
I’m feeling frustrated about the barriers to receiving high quality, publicly funded, trauma informed mental health care. Especially the barriers faced by trans and gender non-conforming folks.
I know that I’m blessed to live in a country that has free universal health care, but we still have a two-tiered system. Psychological care, social work and counseling that happens outside hospital settings is fee-for-service. There are many barriers for those without finances or work place insurance in terms of accessing mental health care. Based on my own experiences, I believe that medication alone should almost never be the first line of treatment for mental illness, and that medication should never be used without corresponding counseling of some type. This does not mean that I’m anti-medication or anti-choice or even fully anti-psychiatry. It just means that I see mental health as more than just a chemical imbalance in the brain. It means that I know that supportive, validating counseling can be helpful in treating most illnesses. I highly value feminist based counseling, intersectional approaches, peer support models and any type of counseling where the patient has a say in what happens and is treated like the expert in their own lives.
I’m personally quite negatively biased against cognitive behavioural therapy. That does not mean that I don’t think it has a place, or that it can never be useful. I believe it can be helpful with certain types of issues, such as OCD. But CBT leaves a LOT to be desired in relation to trauma therapy. It focuses too much on the individual thoughts, feelings and behaviours and too little on trauma, societal oppression and practical barriers.
When I was younger, and I first entered into the mental health care system, my parents found a clinic and doctors that supposedly were experts in the field of eating disorders. Now, maybe they were good doctors, but I can say with absolute certainty that they were not trauma informed. I don’t really remember every being asked exactly WHY I had developed anorexia, or if anything had happened to me.
I’m not an expert, by any means, but I know that young people rarely (if ever) develop eating disorders and self harm just on a whim, out of the blue. Generally eating disorders are symptoms of a larger problem, generally eating behaviours are coping techniques to deal with something.
I was a smart teenager. I knew to some extent why I wasn’t eating. I had learned that it was an effective way to zone out, feel lighter, feel empty and take up less space. I became addicted to that feeling of zoning out, it helped me cope with the sexual abuse I was experiencing. It wasn’t about my looks, it wasn’t about losing weight and it wasn’t about existential angst (per se). I’m not sure if anyone actually ever asked me why I wasn’t eating. And after a certain amount of time had passed, it became irrelevant to everyone. Nobody cared why, they only cared about me eating so I wouldn’t die. I didn’t believe I could die. I’m not sure I REALLY cared if I died. I think I did at that time, but I certainly didn’t care by the time I started taking anti-depressants. I pretty much welcomed the idea of death and started to think about suicide at 17.
These psychologists I went to see worked from a CBT model. I remember being 16 and sitting in the psychologist’s office while he drew diagrams of how thoughts impacted feelings which impacted behaviours which further influenced thoughts and feelings. I quickly picked up on the pattern of it. I realized that a very specific set of responses were the desired outcome. I followed the pattern and started saying what he wanted to hear. I didn’t internalize any of it. It became a game to me, not a game to manipulate or hurt anyone, but a test to see if I said what was expected if I’d be allowed to go back to school and stop missing music class for the appointments (which to me appeared pointless).
Fairly soon after that, I became physically starved to the point my brain wasn’t really working rationally anymore. The physical side effects of the disease confused my brain and the restricting and exercising became obsessive to the point of OCD. The behaviour self perpetuated and I lost track of why I started doing it. I lost track of what happened to me. I lost track of the abuse. I lost track of everything. I felt panicky most of the time. I was always cold.
When someone is that sick, no type of therapy is going to work. Eating is the only treatment. I went to an inpatient program, started the process of weight restoration and my mind gradually cleared. I don’t remember being asked in treatment why I starved myself to the point of near death. I think people were relieved that I was eating and that I returned to some level of semi-normalcy. I was still thin. I still had strange eating habits and anxiety around food. I still avoided eating with most people. But I was well enough to “pass” as recovered.
I began to recover some memories around the age of 18. But they weren’t concrete at first. They were flashbacks, physical reactions, nightmares. I remember talking about it indirectly to my boyfriend at the end of high school. Telling him that something had happened with my last boyfriend. I don’t remember if I shared many details. I think the idea was only slightly formed in my head. I didn’t connect the dots and fully disclose until I was 20.
Then I was thrust into the psychiatric, medical model. I was drugged and drugged and drugged more. The worse I got, the more drugs were given. I was medicated to the point I could barely stay awake during the day time. I felt foggy. I gained weight. I was diagnosed with PTSD, but I still didn’t receive trauma informed care.
I did an inpatient program for PTSD. It helped a LOT. I learned a lot. But I couldn’t fully actualize the learning because I was on too much medication and I was in an abusive unhealthy relationship. I knew by then that the trauma piece was at the centre of my struggles, but I didn’t fully comprehend that my current situation was a major factor.
All this to say, that my life story is a testament to the perils of practicing medicine without considering the impact of trauma on physical and mental health.
I’m so passionate about looking at the roots of why people cope in the ways they do. What societal circumstances and traumas caused them to cope in the ways they do?
Now I’m a parent. My children struggle with anxiety. My younger child is transgender. She has secrets. There are things she won’t talk about to anyone. She struggles with focusing sometimes. I see a lot of signs of trauma and of the impacts of things she has lived through. Experiencing transphobia in and of itself is trauma. Being misgendered, people using her old name, being treated as less than a real girl, being told that her mom is crazy for “forcing her” to be a girl….I could go on, but it’s a lot. A lot for a child. Rejection by a parental figure is one of the clearest predictors of mental illness in trans children and youth. Acceptance is the highest predictor of mental health.
Again. It’s not rocket science. Of course a child will feel safer if they are accepted.
Now I’m the one trying to find the doctors, trying to access the care, trying to get referrals, wait on lists, be taken seriously. 20 years later, I’m still fighting to find a mental health care provider who truly understands the impact of trauma on a child and who is willing to practice trans positive, trauma informed care. I don’t want her forced into CBT. I don’t want her to be medicated. I want someone to help her feel safe enough to express what is on her mind. I want someone to hear why SHE uses the coping she does. I don’t want doctors to guess and assume. I don’t want them to misdiagnose her as well as mis-gendering her.
She deserves to be heard. I don’t want her to be writing a post like this in 20 years.
Kids will say what they think adults want to hear. They may do it consciously, or unconsciously or for their own reasons. They do it to please, to stay safe, to feel a sense of control and many other reasons. It takes a special type of doctor or counselor to help a child feel safe enough to tell their truth. Because after enough time hiding, even she will be confused about what her truth is.
Mental health care for children should be free. The practitioners should be trauma informed. There should be enough funding that kids can access the care they need without lengthy wait lists. There should not be a two tiered system where those who can pay can access things those in poverty cannot. Poverty is a risk factor as it is, without it also limiting access to care. Ideally there should be a system that is easier to navigate, where parents don’t feel they are fighting and advocating to the point of exhaustion.
Mental health care is a right, not a privilege.
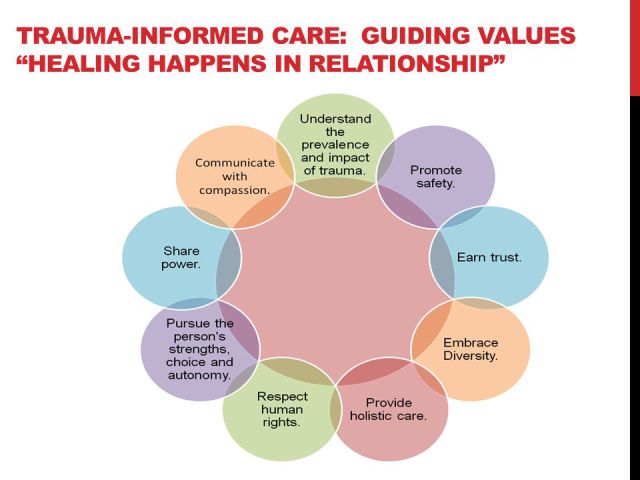
Photo: https://makingmomentsmeaningful.blog/2017/04/13/trauma-informed-care-values-youth-worker-values/
I so want that for your child too! To be heard and to be validated and not forced into any therapy or medication that does not feel right.
I agree with you on the OCD CBT but that CBT is not right for trauma. In my experience. I know this guy who swears by it and says it was the only thing that worked for him. It is not something that I would think would be good for trauma. Forced to do something or not do something that was a coping skill. Just doesn’t make sense to me.
I also find myself searching the root of why I myself coped the way I did.
I know that having accepting parents is crucial in healthy mental health. It is one stepping stone towards accepting yourself.
LikeLike