It’s been a long time since I’ve written a blog post. Even tonight as I sit down to type this, I’m not clear on what I’m going to write about.
I’ve been focused on my children and my family for the last few months. It’s been difficult to connect or find the energy to do much other than collapse on the couch to watch Netflix at the end of each busy day. I have my children with me full time now. Their father moved to another part of the country and they haven’t seen him since October. He didn’t plan a visit for Christmas.
We are all of us coping with this abandonment in different ways.
For me, there has been an incredible amount of anger.
I don’t feel comfortable in the anger. I don’t feel comfortable with how little patience I have and how quickly I snap at people or shut them out if they cross a line from support into offering advice. I’ve isolated myself more than usual.
The anger is just barely covering a deep well of sadness and fear. Sometimes I feel completely overwhelmed with the amount of trauma my small family has endured in the past few years. I worry about the impact it will have on my children. I worry about not having the right help for them. I worry about not being patient enough. I worry about being a solo parent, all the responsibility on me. I worry about the lifelong impact of parental abandonment after years of emotional abuse and neglect.
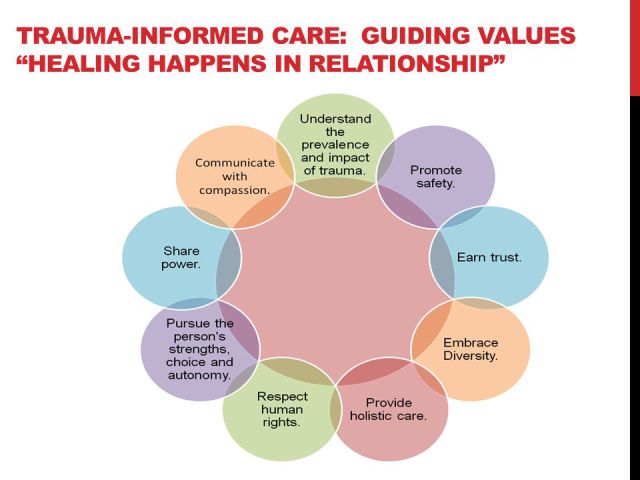
I think about the research that has been done about adverse childhood experiences (ACEs) in relation to trauma theory and the negative impact on health. For those who might not be familiar with the research, here is a visual representation:
My kids have experienced emotional abuse and neglect and physical neglect at times. I don’t know for certain about physical and sexual abuse. I may never know. They have a parent with a mental illness. Their parents are divorced and their mother is a survivor of family violence. There is a history of substance abuse on both sides of their family (though not with either parent).
I try not to think about it. I try to think about the research on resilience which shows that if children have even one positive, consistent and stable adult in their life, it mitigates the impact of ACEs. I try to believe. I need to believe it is true in order to function on a daily basis, rather than fall into a pit of hopeless despair.
My older child was recently diagnosed with learning disabilities. This did not come as a surprise to me. For two years her father refused to consent for the testing to be re-done. Earlier testing had been inconclusive for a number of reasons and it was recommended to be repeated. He refused to agree. He denied she had any learning issues and blamed me for instilling anxiety in both my children.
Yesterday, as I listened to the feedback from the psychologist. I heard her saying again and again how different aspects of the test results, including some of the discrepancies between the recent and prior testing, could be linked to the impact of trauma on a developing brain.
Essentially, she was talking about the impact of ACEs on my child’s brain.
I felt numb. What reaction is normal? How can a caring parent just accept these things? How to function and keep moving forward, filled with the knowledge that my kids have experienced trauma?
Intellectually, I know it isn’t my fault. I know I’ve done the best I could. But the dark voice inside tells me that it is my fault. That I never should have had children. That someone with a mental illness like mine should never have been a mother. That I never should have had children with an abusive partner. That I should have left him sooner. That I should have stayed with him to protect the kids…
All the ways…all the blame.
I push it all down. Try to keep busy. Try to block out the thoughts and worries. Turn on the TV. Pick up my cell phone. Browse the internet mindlessly for hours.
In the evening, I feel a sense of panic. I’m a fraud. I’m not capable. I find myself thinking old thoughts, falling back into old thought patterns. “I can escape my responsibilities by hurting myself” and “It’s too hard. I can’t do it. I’m a failure” I think about self harm and suicide. Then berate myself for how literally insane it is. I can’t die. I’m simultaneously gripped in a tight knot of constant fear and terror about dying and leaving my kids alone with their father, and desperate to escape from a life that often feels TOO painful to endure. I think about suicide and actively wish I was not alive, while at the same time worrying about getting sick or having an accident, and the consequences on my children if I’m not here 100% of the time and 100% functional.
It’s exhausting. I honestly want to sleep and watch TV, curled in warm blankets, for many days. I want to escape from SO much responsibility. But I can’t. I get up each day, and I function. I do ALL the things. I keep going, because I have to.
My mind is a bit all over the place recently. Instead of having a certain set of trauma memories and flashbacks which bother me consistently, I have been experiencing mixed up flashes of a whole spread of my traumatic experiences. Memories popping into my mind, unexpectedly, and me pushing them back down again.
I started a new job, teaching a course at the university I went to during the years before my separation. Going back to the campus brought back memories of those two years, when I was so unwell, cutting myself and ending up in the emergency room on a regular basis. I received ECT the week I completed my last semester. I felt depressed and trapped and I hadn’t yet made the connection to my abusive marriage. During those years, it was still JUST ME. I felt like I’d exhausted every treatment option and I was ready to give up. I wrote a post-it note suicide notes to my children but then went to the hospital and had my injuries treated. I felt like I was falling into pieces and not able to put them together again. I never felt calm or safe. I had nightmares and woke up screaming and trying to escape from imagined abusers.
My brain also dredged up memories and flashbacks of the undergraduate professor who sexually assaulted me in my apartment, less than a year after my graduation. It happened in December. I sat frozen on my couch while he touched me. I didn’t fight back, I didn’t say no. I just froze and disassociated, my eyes fixed on his black and gold scarf. I was powerless to stop him. The only reason it ended was that at some point he noticed that I was completely gone and even he didn’t want to touch a statue. It took what felt like hours before I could even speak to ask him to leave. I remember crying, but as a statue would cry, tears moving over a frozen face.
In a way, I feel safer now that my ex-husband doesn’t live in the city. But I still tense up when I see a car like his. I still get jumpy at night sometimes, thinking I hear someone in the house. I still get anxious about something happening to the kids, even a minor injury, that he might get angry about. I am in equal parts afraid he will respond to my mandatory email updates about the children, and furious that he ignores me so completely. I feel at the same time invisible and caged. I feel trapped in a cage.
The cage of abuse and trauma. I don’t know how to escape and I don’t know how to release my children from the cage either. When abuse has gone on for so long, the abuser doesn’t even have to be in the same city, or have contact with you, to control you with the fear of what MIGHT happen. The bars of the cage are memories, fears, and what ifs. The fear alone is enough to modulate our behaviour, even with little or no contact from him.
I’m tired. I get tired of hearing myself say that I’m tired. But I’m tired. I’m always tired.
Yes, there are good days and things to be thankful for. This post isn’t ungrateful or dismissive of the blessings in my life. It’s more to say that no matter how bright the joys and how wonderful the blessing, I still feel caged. I still wonder how it can be possible to “live a normal life” or “be healed” or “recovered” after so much trauma.
I know it’s possible. I know that ACEs aren’t a death sentence. I know that our family has a lot of support, a lot of strengths and a lot of STRENGTH.
But some days PTSD makes it hard to be optimistic. Is a bird in a cage optimistic about escaping? Or in captivity do they gradually stop singing and lose their vibrancy? A bird doesn’t belong in a cage.
And neither do I.